The Diagnosis of Autoimmune Pancreatitis
While there is no cure for autoimmune pancreatitis, some treatments are available to help manage the symptoms. The primary treatment is corticosteroids, which help to reduce inflammation and calm the overactive immune system. The dosage is typically very high but can be tapered off over time. Additional treatments may be needed if complications occur, such as the narrowing of the ducts. Fortunately, autoimmune pancreatitis does not affect the patient's life expectancy.
Type 1 autoimmune pancreatitis
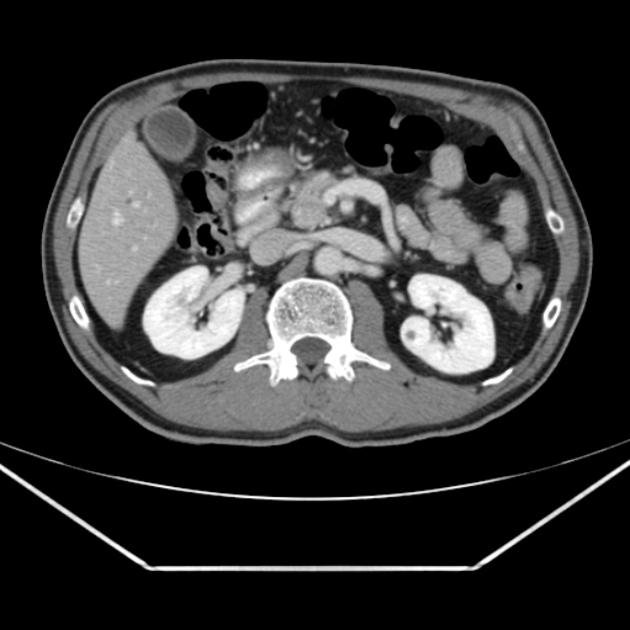
Although Type 1 autoimmune pancreatitis symptoms can vary greatly, there are several ways to diagnose it. First, your doctor may recommend imaging tests, biopsy, or both, to help pinpoint the exact cause of the condition. Imaging tests usually include a CT or MRI scan, although ultrasound may also be used to examine the pancreas. The biopsy, meanwhile, involves the collection of a sample of pancreatic tissue that is examined for signs of autoimmune activity. Sometimes, your doctor may suggest a corticosteroid trial to help confirm your diagnosis. Taking short-term steroids can lower IgG4 levels and improve imaging findings.
Yoshida and colleagues first proposed the concept of autoimmune pancreatitis (AIP) in 1995, and it has since gained widespread recognition as a distinct pancreatic inflammatory disorder. Recent studies have identified two subtypes of AIP, type 1 and type 2. Type 1 is characterized by an increased serum IgG4 concentration and granulocytic epithelial lesions.
Relapse rates
Relapse rates of autoimmune pancreatitis (AIP) are high, but factors that predict relapse are not well defined. Some studies have shown that factors such as diffuse type IgG4 seropositivity and jaundice are not predictive of relapse. However, these factors are assessed at diagnosis and do not reflect the course of treatment.
The disease has two main subtypes: type I and type II. Type I has a high prevalence in males, whereas type II does not show a gender bias. Type II patients do not have an elevated serum IgG4 level and do not typically have other organ involvement. According to a recent multicenter analysis, the average age of patients diagnosed with either type was 61.4 years in type 1 and 39.5 years in type II. In type 1 patients, the proportion of males was 77%.
Causes
A diagnosis of autoimmune pancreatitis requires a variety of diagnostic tests. These tests will help identify abnormal IgG4 levels and may check liver function or the levels of certain blood cells. In some cases, a biopsy of the pancreas will also be necessary. The biopsy may be obtained using an endoscopic ultrasound or a small incision in the skin. Other tests may include blood tests or imaging tests.
Autoimmune pancreatitis is characterized by a diffusely enlarged pancreas and a high IgG4 level. Symptoms often respond well to steroid therapy. However, patients should seek medical advice if their symptoms persist despite corticosteroid therapy. In addition, patients with this condition should not confuse it with other states, including chronic pancreatitis and pancreatic cancer.
Diagnosis
Diagnosis of autoimmune pancreatic disease (APD) is difficult and complex. This rare, fibroinflammatory disease accounts for approximately five to six percent of all cases of chronic pancreatitis. In most cases, this disease responds well to steroid treatment.
There are two major subtypes of autoimmune pancreatitis. Type 1 is associated with elevated serum IgG4 levels and is characterized by tissue invasion by plasma cells. Other symptoms include lymphoplasmacytic infiltration, storiform fibrosis, and obliterative phlebitis. Other autoimmune diseases often accompany both types of autoimmune pancreatitis, and type 1 is more prevalent than type 2.




