Systemic Lupus
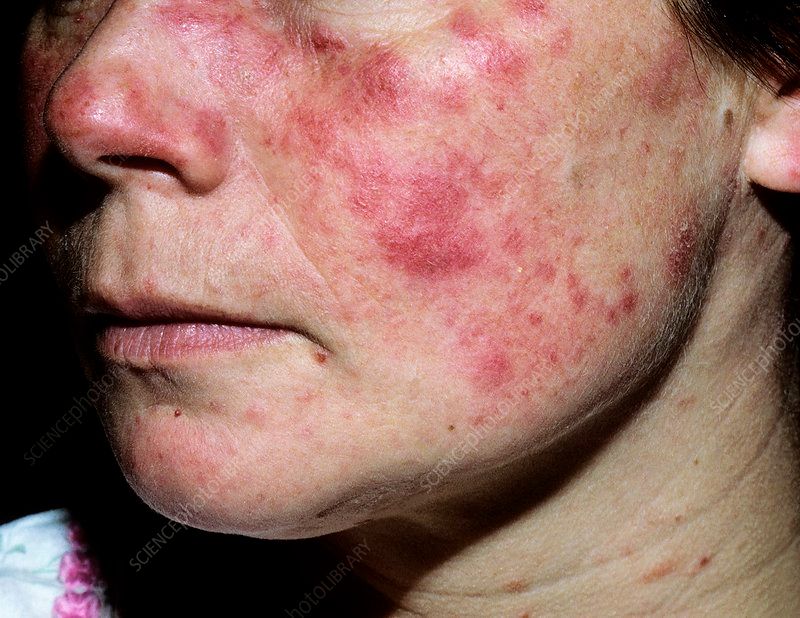
Systemic lupus is a chronic disease that affects the body's tissues and organs. A variety of symptoms and features characterizes it. Lesions, clinical features, classification, and treatment options are discussed. Learn more about systemic lupus by reading this article.
Lesions
Systemic lupus erythematosus (SLE) is a chronic multisystem inflammatory disease with autoimmune aetiology, which is more common in women than men. The disease can be easily diagnosed through clinical features, and the condition is treated with corticosteroids.
Common symptoms of systemic lupus include painful cutaneous lesions and subcutaneous lesions. The skin lesions are typically erythematous to violaceous in colour and often result in scarring or atrophy. Other symptoms of systemic lupus erythematosus include subcutaneous nodules, lupus panniculitis, and lupus erythematosus.
Clinical features
Systemic lupus erythematosus (SLE) is an autoimmune disease that affects multiple organs and systems. It is triggered by an abnormal immune response caused by genetic and environmental factors. The symptoms of SLE can range from skin and joint inflammation to serious organ involvement. Most cases occur in women. Women are most likely to develop SLE before age 18, and men are more likely to develop the disease after age 50.
Clinical features of SLE are very varied, with many patients presenting with only one or two symptoms. The most common presenting manifestations are cutaneous and constitutional, which are present in half of the lupus patients at the time of diagnosis. However, patients may present with several other clinical features that may be the first clues to diagnosing the condition.
Classification
The ELRA/American College of Rheumatology has published updated criteria for systemic lupus erythematosus (SLE). These criteria are based on a cluster of clinical findings and laboratory evidence. They help clinicians identify and subclassify the disease according to its target organ manifestations.
The new EULAR/ACR SLE classification criteria, which include the presence of at least one positive ANA, constitute a paradigm shift in the classification of SLE. In addition, its sensitivity and specificity are high, with 96% sensitivity and 93.4% specificity, making it an important tool for clinicians and researchers.
Treatment
Treating systemic lupus begins with a visit to your primary care doctor, who may refer you to a rheumatologist for further diagnosis. However, because lupus symptoms can be similar to those of other illnesses, your doctor will need to rule out other causes of your symptoms before recommending a treatment plan. This may involve referring you to a kidney specialist, a blood disorder specialist, and even a neurological disorder specialist.




