Pancreatic Ductal Cells
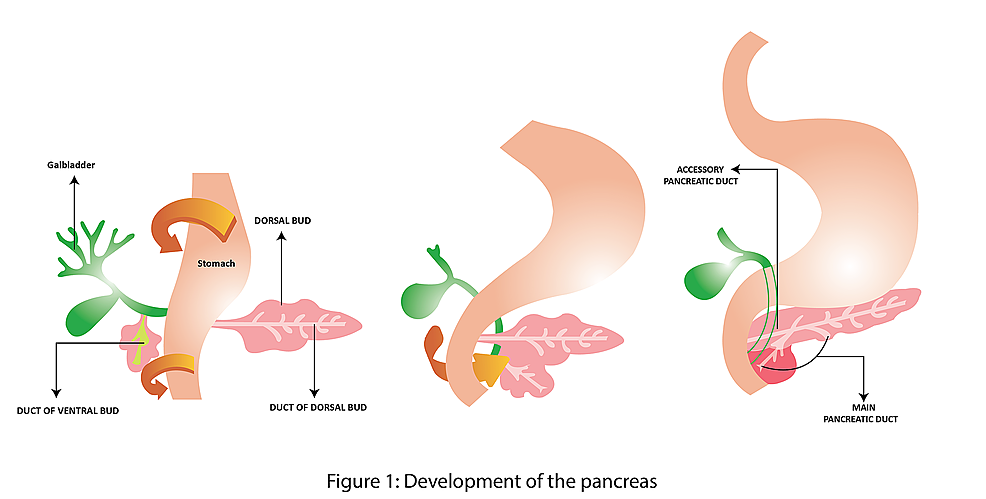
The ductal cells of the pancreas exhibit morphologic heterogeneity along the length of the acinus. The duct cells closest to the acinus are squamous, with very few cytoplasmic vesicles and numerous mitochondria. These morphological features correspond to different modes of fluid transport, whereas the cells further distal to the acinus are more rounded with more cytoplasmic granules and vesicles and secrete proteins. These differences correlate with the morphological characteristics of solute-transport proteins.
Endocrine
The pancreas is a gland containing both endocrine and exocrine glandular tissue. Exocrine tissue makes up 99 percent of the pancreas, while endocrine tissue comprises the remaining 1%. Exocrine cells are grouped in acini clusters and secrete digestive enzymes. The ducts of these acini merge to form the pancreatic duct. The pancreatic duct delivers these digestive enzymes to the duodenum.
Centroacinar cells
Pancreatic ducts consist of two main elements: the intra-acinar and the intercalated duct. The intra-acinar ducts are composed of flat or cuboidal epithelia that connect to form the acini. The intercalated ducts connect to form the larger, intralobular ducts. The larger interlobular ducts are lined with columnar epithelia. Centroacinar cells line the interlobular ducts, which branch off into 20 branch ducts. The latter empties into the main pancreatic duct.
Goblet cells
In a hamster, the pancreatic ductal goblet cells can be considered a model for human mucus-secreting cells. Goblet cells are simple columnar epithelial cells that secrete gel-forming mucins and vesicles. When stressed, they also secrete by apocrine means. The cells can be identified by their goblet-like shape, with an apical portion that resembles a cup and a basal section that lacks granules.
Intraductal papillary mucinous neoplasm
Intraductal papillary mukineoplasm (IPMN) is a morphologically and biologically heterogeneous group of neoplasms of the pancreas. This study aims to evaluate the clinical features and survival of invasive IPMN and background IPMN. The study cohort included 61 patients with invasive IPMN and 570 with pancreatic ductal adenocarcinoma. The authors used a stage-matched Cox proportional hazard model to analyze the prognosis.
Pancreatic duct
Although the natural growth rate of pancreatic ductal carcinomas is unknown, studies have demonstrated a rapid progression of these tumors. The 7-mm pancreatic duct adenocarcinoma mass increased to 13 mm in about 22 months. This mass required surgical resection. The survival rate of patients with this type of tumor is about 80 percent. However, the prognosis is not as favorable as that of invasive pancreatic ductal cancer.




