Pancreatic Cancer Diagnosis
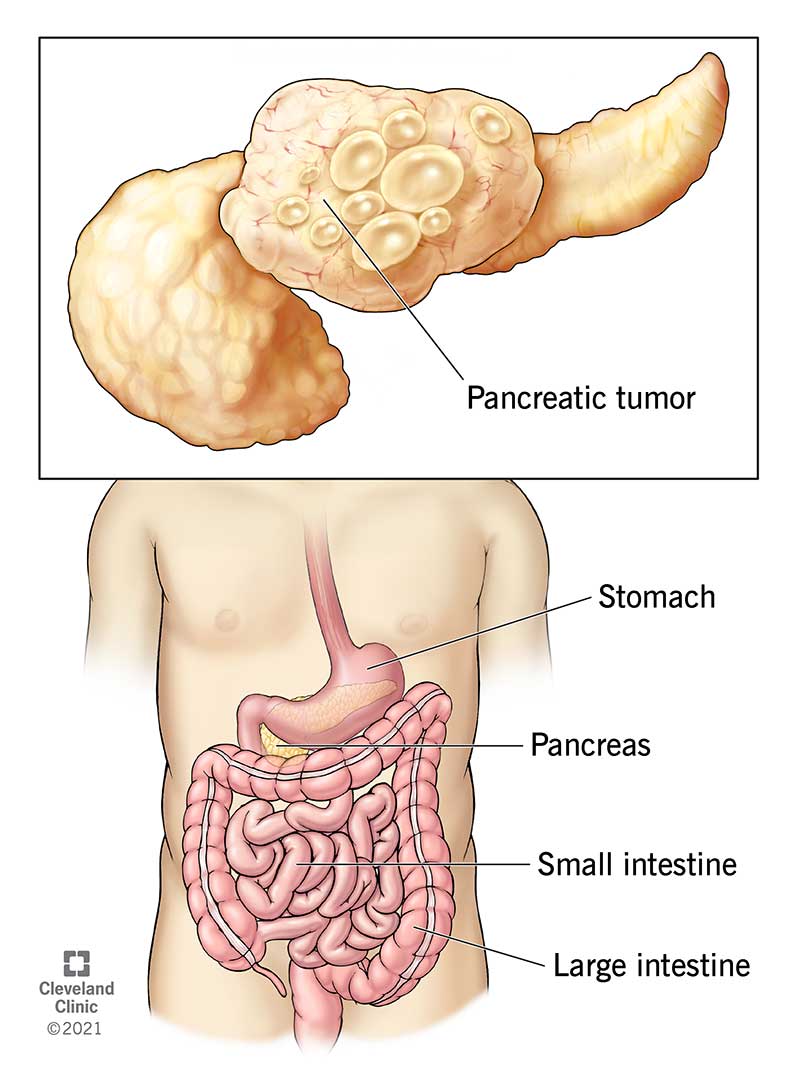
Cancer of the pancreas has several stages. Stage 2A pancreatic cancer, for example, is larger than four centimeters in diameter and has spread to at least three lymph nodes. This type of cancer can often be cured with surgery and a combination of treatment options. Earlier stages of pancreatic cancer do not cause noticeable symptoms. For this reason, surgery may be a viable treatment option.
CT scan
A CT scan is a diagnostic test used to determine the presence of cancer in the pancreas. It works by combining powerful magnets and X-ray equipment to create multiple images of the internal organ. This test can detect whether pancreatic cancer has spread to nearby lymph nodes and the liver. Doctors also use this test to monitor the progress of a pancreatic cancer patient after treatment. The scan can help them determine whether cancer has spread or recurred or whether it has metastasized.
MRI
An MRI for pancreatic cancer diagnosis is a diagnostic imaging procedure that uses radio waves and powerful magnets to create detailed 3-dimensional images of the body. The scan produces images in slices extending across the body's length and can help doctors determine the extent of cancer. The image can be used to help doctors decide on the type of treatment to begin. The procedure typically takes one to 1.5 hours and requires the patient to remain still.
Biopsy
A biopsy is the most definitive way to diagnose pancreatic cancer. Various techniques are used to obtain tissue for histological assessment. A biopsy during an ERCP can help doctors identify whether or not you have the disease. For example, Kubota and colleagues used biopsy forceps to collect transpapillary tissue from 43 patients. Tissues were adequate for evaluation in 95.3% of cases. The biopsy is sometimes combined with brush cytology and intrapancreatic ductal endosomal to improve its accuracy.
Blood chemistry tests
Pancreatic cancer is one of the most deadly types of cancer, and it is expected to become the second-leading cause of cancer in the United States by 2030. A new blood test may be able to diagnose pancreatic cancer at its earliest stages when it's most likely to respond to treatment. The test measures the levels of two specific proteins in the blood. It accurately separates tissue samples from patients with pancreatic cancer from those with non-cancerous conditions.
Image-guided biopsies
An image-guided biopsy is an important step in pancreatic cancer diagnosis. The process can improve the accuracy of diagnostic tests by eliminating unnecessary steps. Currently, the most common imaging modality used during pancreatic biopsies is CT. However, other imaging modalities such as MRI, ultrasound, and magnetic resonance imaging (MRI) are also available. The advantages of image-guided biopsies are obvious: they provide real-time imaging, are less invasive, and use no ionizing radiation.
Moreover, image-guided biopsies are less costly than CT. However, some downsides remain. The pancreas is posteriorly, and the needle tip can be hard to visualize.
Molecular testing
In addition to imaging tests, a physician may use a variety of diagnostic tests to find the exact cause of pancreatic cancer. These tests will help your doctor determine the disease's stage and how much of the tumor is cancerous. Your doctor will ask you about your medical history and any risk factors for developing cancer. A biopsy of the tumor will be necessary to confirm a diagnosis. A tumor biopsy may also reveal other symptoms, including pain, inflammation, and anemia.



