Autoimmune Gastritis
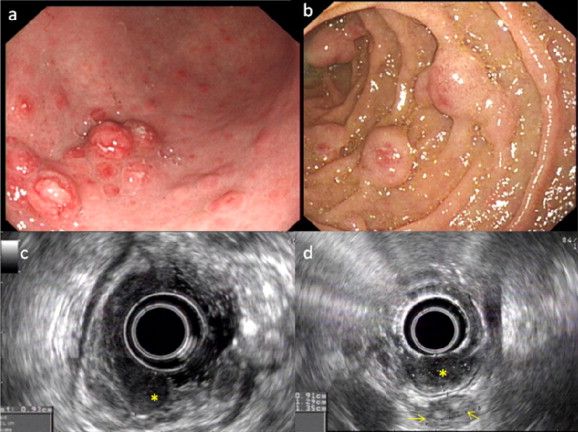
Autoimmune gastritis is an inflammatory disorder that affects the gastrointestinal tract. In a 2012 observational study, more than half of patients with autoimmune gastritis also had one or more other autoimmune conditions. These included type-1 diabetes, Hashimoto's thyroiditis, celiac disease, rheumatoid arthritis, and Grave's disease. Many autoimmune diseases share a common thread: disruption of the gut microbiome.
Metaplastic (chronic) atrophic gastritis
Metaplastic (chronic) atrophic gastritis is a disease affecting the gastric tract's mucosa and epithelium. The main features of this disease include thinning of the gastric mucosa and loss of epithelial cells. Patients with this disease are also at risk for gastric dysplasia.
The most reliable method to diagnose metaplastic atrophic gastritis is biopsy with subsequent histology. However, there are limitations in interpreting histological findings in the early stages of the disease. Nevertheless, histological findings of atrophic gastritis may reveal it infiltrates plasma and lymphocytes. In addition, atypical morphology of the oxyntic mucosa may be present.
Multifocal atrophic gastritis
Multifocal atrophic gastric lesions are considered precancerous, as they can lead to gastric cancer. The condition is most common in places with overcrowding or extreme poverty. The doctor may also perform an endoscope biopsy to identify the cause of symptoms. The presence of Helicobacter pylori is a common cause of atrophic gastritis.
In addition to precancerous lesions, atrophic gastritis can lead to complications such as gastric cancer and micronutrient deficiencies. It can also cause problems with erythropoiesis. This review aims to provide an updated overview of the epidemiological, clinical, and therapeutic aspects of atrophic gastritis.
Non-autoimmune gastritis
Non-autoimmune gastritis occurs when a specific autoimmune process does not affect the stomach. The symptoms of this condition are similar to those of other autoimmune disorders. However, they involve inflammation of the parietal cells. These cells secrete gastric acid and intrinsic factors. Non-autoimmune gastritis can be a chronic condition that progresses over time. In some cases, the state can go to the point of neuroendocrine disease or iron deficiency.
Although no definitive cause of non-autoimmune gastritis has been identified, several triggers perpetuate the symptoms of this condition. One such trigger is using certain drugs or NSAIDs, which damage the stomach lining. This breaks down the protective barrier, which leads to further inflammation.
Polyglandular autoimmune syndrome type IIIb
Polyglandular autoimmune syndrome type IIIB is a genetically inherited condition that affects the glands. The etiology of this disorder is not fully understood. However, several factors can trigger the disease. Listed below are some of them.
Polyglandular autoimmune syndrome type IIIB is associated with several autoimmune disorders, including autoimmune thyroiditis. The condition can also occur in patients with alopecia and vitiligo. In addition, the syndrome may also be associated with diabetes mellitus and autoimmune thyroid disease.




