Antiphospholipid Syndrome
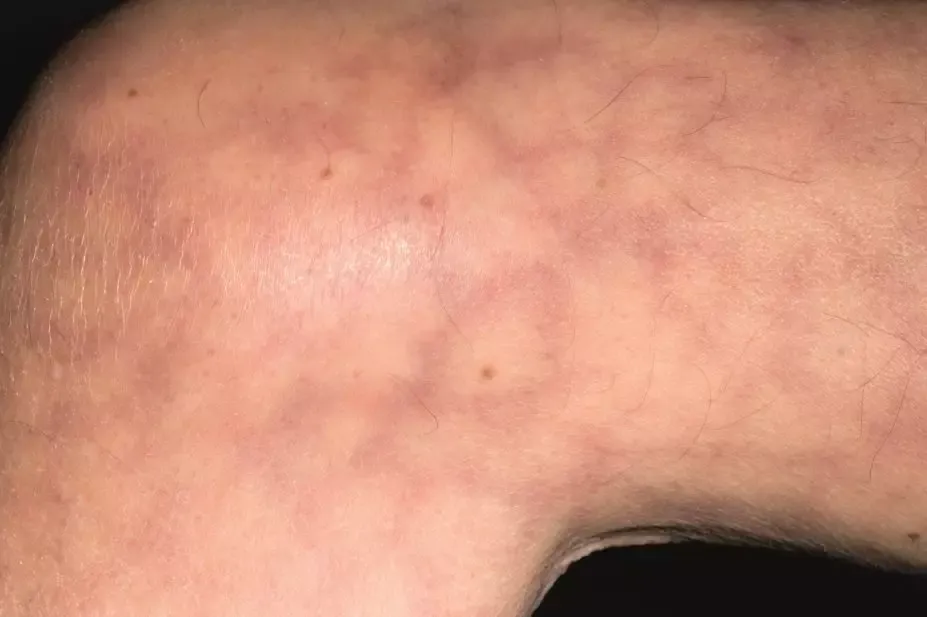
Antiphospholipid syndrome diagnoses are based on a detailed clinical examination and patient history. The condition is often characterized by at least one blood clot. Several blood tests can be used to confirm the diagnosis. However, in some cases, a simple blood test is sufficient for the diagnosis.
Thrombocytopenia
Thrombosis is a common complication of Antiphospholipid Syndrome (APS). Antiphospholipid antibodies attack b2-glycoprotein I, a protein found in the lining of blood vessels. These antibodies can cause hypercoagulability and lead to arterial thrombosis. Antiphospholipid antibodies can be directly or indirectly bound to platelets.
The diagnosis of APS is based on a careful clinical examination and detailed patient history. A physician may order a blood test to determine if the condition is present. Some patients experience bleeding from the nose, gums, or skin. Other symptoms of APS include unusually heavy menstrual periods. Occasionally, blood clots can form in the brain, causing numbness and pain.
Placental abnormalities
Antiphospholipid antibodies are one of the major causes of fetal wastage. According to Ware Branch, women with APS experience more than 70 percent fetal wastage. This figure is significantly higher than the 10 percent reported by women with normal antiphospholipid antibodies. Furthermore, women with APS are at a higher risk for recurrent fetal wastage.
Placental insufficiency in women with primary APS is a common complication of the disorder. This can lead to intrauterine growth restriction, pre-eclampsia, premature delivery, and thrombosis. In this study, researchers looked for macrophage infiltration signs and placental trophoblasts in women with treated primary APS and controls. They examined trophoblasts by immunohistochemical methods, such as periodic acid-Schiff stain, alpha-actin, and VCAM-1.
Blood clots
Antiphospholipid syndrome is a relatively common cause of venous thrombosis. About 20% of cases of deep vein thrombosis are associated with antiphospholipid antibodies. These antibodies are typically detected in lupus anticoagulant assays or anticardiolipin assays. They are directed against phospholipid-binding plasma proteins, including b2-glycoprotein I and prothrombin. The presence of antiphospholipid antibodies has been linked to hypercoagulability in various animal models and in vitro studies. Therefore, patients with antiphospholipid syndrome should undergo long-term anticoagulation to prevent recurrent venous thrombosis.
Blood clots caused by APS are particularly dangerous. They can block blood flow and damage heart valves. They can cause symptoms such as chest pain and difficulty breathing. They can also result in a heart attack. Patients with APS may also have a reduced platelet count and a condition called thrombocytopenia.
Heart valve abnormalities
Heart valve abnormalities due to the antiphospholipid syndrome are associated with an increased risk of thrombotic and bleeding complications. Patients with APS also face greater surgical risk. In one case, a patient with APS underwent cardiac valve replacement surgery and developed a severe thrombotic event. Although the patient eventually recovered, the case raised important questions about the role of APS in cardiac valve surgery.
Patients with antiphospholipid syndrome have an increased risk of thrombosis, especially arterial thrombosis. A recent case report describes a young patient who developed chest pain and was found to have coronary embolism related to aortic valve thrombosis. Cardiovascular MR imaging was used to make the diagnosis.
Genetics
The genetics of antiphospholipid syndrome (APS) is still under investigation. There are several theories based on which the disease can be inherited. Some of these theories are related to immune responses, while others are related to phospholipid metabolism. Thus, the study of selected SNPs could provide new clues to the pathogenesis of APS.
One hypothesis relates to the production of antiphospholipid antibodies (aPLs). APS is an autoimmune disease that can lead to recurrent pregnancy loss, thrombosis, and heart failure. Although genetics play a role in the development of APS, environmental factors may also influence the disease's development. Infections, such as bacteria and viruses, have been implicated in initiating autoimmune responses, which can lead to many complications.




